https://images.app.goo.gl/Dmq1nMY8PkBBmDu48
Considering that the mind and body are interconnected by a complex network of neural circuitry, autonomic dysregulation is an interesting way of looking at overall mental and physical health.
Autonomic nervous system (ANS) symptom patterns that involve the cardiovascular, respiratory, gastrointestinal (GI), urogenital, and dermatologic systems are described as autonomic arousal disorders and can lead many people to seeking help for vague physical symptoms that don’t seem to have the underpinnings of a standard illness or medical condition.
The DSM-5 details the category “Other Specified or Unspecified Somatic Symptom Disorder” to describe mental and physical symptoms that persist at least 6 months and are below the threshold for the diagnosis of a specific illness. The symptoms are not caused by, or fully explained, by another medical psychiatric, or substance use disorder, and they cause significant distress or impairment (Sadock, et. al, 2018; APA, 2013). Unbalanced stimulation of either the sympathetic or parasympathetic system with problems in the feed-back loop of neurotransmitters such as norepinephrine and acetylcholine can cause symptoms such as, racing heartbeat, shortness of breath, yawning, cramping and diarrhea, nausea, flushing, pruritis or rashes, urinary frequency, and chronic, non-specific reports of pain and fatigue.
The implication that autonomic dysfunction plays a part in mental and physical health is an area of ongoing study. There is an association between hypertension, heart disease and anxiety, particularly related to psychosocial stressors, due to the autonomic arousal via the hypothalamic-pituitary axis (HPA) which stimulates the sympathetic system and increases circulating catecholamines. As Player & Peterson discussed in a 2011 review article, the heightened arousal with sympathetic stimulation is “associated with an increased risk of hypertension and a pro-inflammatory state and, consequently, development of coronary heart disease.” They note that other studies show links between panic disorder and PTSD, and adverse cardiovascular outcomes. Autonomic dysfunction disrupts hormonal balance, as well, which can lead to further inflammation, metabolic abnormalities and insulin resistance (Player & Peterson, 2011).
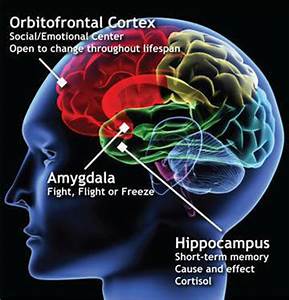
In 2016, researchers published a study in Biological Psychiatry on the alterations in amygdala-prefrontal brain connectivity and the relationship with autonomic dysregulation. Their participants were diagnosed with generalized anxiety disorder (GAD) who demonstrated excessive worry, the core symptom of GAD. The researchers describe the dysregulation seen in GAD as the inability to control worrisome thoughts and the “chronic failure to down-regulate autonomic arousal”. During stress, medial prefrontal cortices and the amygdala are activated. Changes in parasympathetic/sympathetic tone causes baroreflex suppression that results in an increased heart rate (HR) and blood pressure and a decrease in HR variability (HRV). They note that decreased HRV is a characteristic of autonomic dysfunction in those with GAD. Functional magnetic resonance imaging (fMRI) studies link excessive worry to abnormal connectivity between the amygdala and prefrontal cortex and that people with GAD exhibit typical patterns of autonomic dysregulation, such as increased heart rate and breathing and/or GI symptoms, that implicate alterations in the fronto-limbic circuitry. Their study looked at the association between the core symptoms of GAD and autonomic dysregulation and found that they arise from a shared underlying neural mechanism (Makovac, et.al, 2016).
Many clients who report to me that they are not feeling “right”, finding themselves somewhat irritable and on edge, with feelings that they are short of breath and that their heart is sometimes “pounding” out of their chest, state that the “attacks” are often random and without a notable trigger. Many clients also report feeling overwhelmed and lacking motivation and energy. Caffeine and sugar are often used as stimulants. Sleep and focus are often impaired. While daily medication has its place in an overall treatment plan, learning to augment one’s own mind-body connection by affecting the power balance of the ANS with the consistent use of stress reduction techniques such as breathing techniques, exercise, good nutrition, good sleep, and by employing eastern modalities such as acupuncture, yoga and meditation, is important as well.
Everything in our body attempts to be in balance by feedback loops. The concept that the body is simply manifesting physical symptoms of an imbalance between the sympathetic and parasympathetic systems is interesting and worth exploring!

References
American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders: DSM-5 (5th ed.). Washington, D.C: APA.
Makovac, E., Meeten, F., Watson, D. R., Herman, A., Garfinkel, S. N., D. Critchley, H., & Ottaviani, C. (2016). Alterations in Amygdala-Prefrontal Functional Connectivity Account for Excessive Worry and Autonomic Dysregulation in Generalized Anxiety Disorder. Biological Psychiatry, 80(10), 786–795. doi:10.1016/j.biopsych.2015.10.013
Player MS, Peterson LE (2011): Anxiety disorders, hypertension, and cardiovascular risk: a review. Int J Psychiatry Med 41:365–37.
Sadock, B.J., Sadock, V.A., & Ahmad, S. (2018). Kaplan & Sadock’s pocket handbook of clinical psychiatry (6th ed.). LWW.